9 results
An infection prevention and control program established in the wake of the Ebola epidemic: Where are we, and how well are we doing?
- Bobson Fofanah, Christiana Conteh, Victoria Katawera, Ibrahim Franklyn Kamara
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, p. s76
-
- Article
-
- You have access Access
- Open access
- Export citation
-
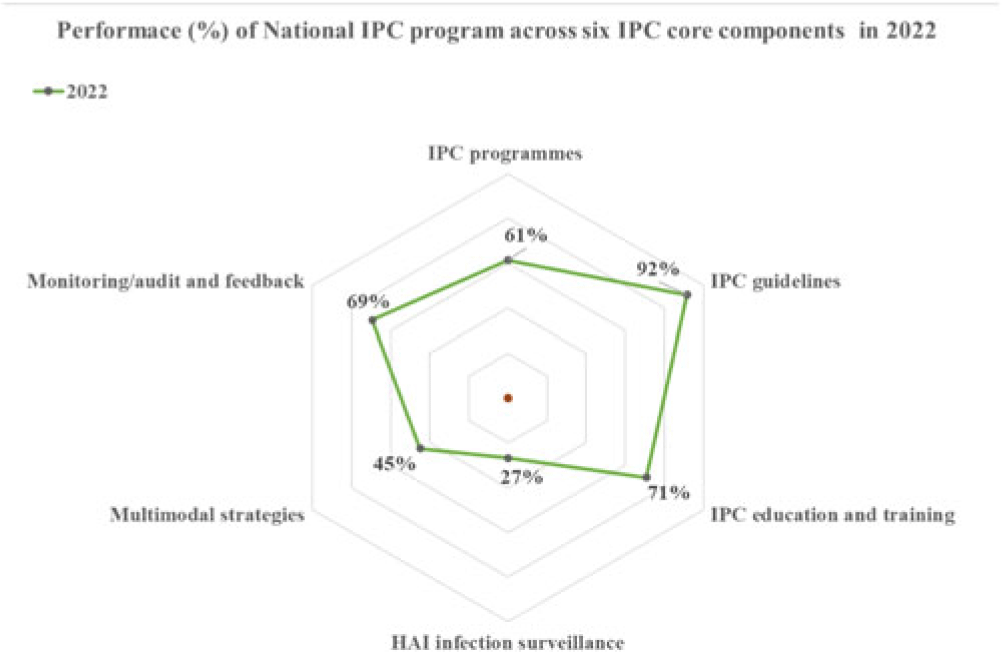
Background: Infection prevention and control (IPC) is a clinical and public health discipline based on a scientific approach and practical preventive and control measures. During the 2014–2016 West African Ebola outbreak, the high number of healthcare worker infections was attributed to inadequate IPC in Sierra Leone. This stimulated the establishment of national and subnational IPC programs. Since then, IPC has remained a priority to improve the health systems and strategic interventions during public health emergencies. Therefore, we conducted a detailed review to assess the status of the IPC programs. Methods: A descriptive analysis of the status of IPC programs in Sierra Leone was done using data from IPC assessments conducted in 2022 by the national IPC team, reviews of reports on program implementation, and experts’ objective opinions. Results: Performance. The national IPC assessment revealed strengths in 4 of 6 WHO IPC core components, with an overall score of 61% positioned at the ‘intermediate’ level of implementation. The best-performing component was ‘IPC guidelines’ (92%) with evidenced-based guidelines being developed and implemented over the years. Secondly, ‘Education and training’ (71%) made progress in basic and advanced IPC training, including the development of a preservice training curriculum. Also, ‘monitoring and audit and feedback’ (69%) and ‘IPC program’ (61%) met the basic requirements of an established Monitoring & Evaluation (M&E) system. Similar progress was made at the healthcare facility level, but with major gaps in ‘workload, staffing, bed-occupancy’ and ‘safe or built environment.’ Sustainability efforts. Evidence-based data on IPC have always been scarce due to a limited capacity to conduct IPC research. The Structured Operational Research and Training Initiative (SORT-IT) on antimicrobial resistance has helped promote evidence-informed decisions and build OR capacity that is relevant to improving program performance. In 2019, Sierra Leone instituted in-country production of alcohol-based handrub and liquid soap as a strategic intervention for providing hand hygiene products for use in healthcare facilities. This intervention was essential during the peak of the COVID-19 pandemic. Although most aspects of IPC implementation are government led with strong leadership support, stable funding and sustainability planning are yet to be achieved and will be crucial for long-term success. Conclusions: Most aspects of the IPC core components have been well implemented at the national level since the establishment of the IPC program. However, the program should continue improving the scope and quality of implementation and focus on the development of long-term plans to sustain existing gains and further improve on gap areas at the national level and especially the healthcare-facility level.
Disclosures: None
High levels of surgical antibiotic prophylaxis: Implications for hospital-based antibiotic stewardship in Sierra Leone
- Sulaiman Lakoh, Joseph Sam Kanu, Sarah K. Conteh, James B.W. Russell, Stephen Sevalie, Christine Ellen Elleanor Williams, Umu Barrie, Aminata Kadie Kabia, Fatmata Conteh, Mohamed Boie Jalloh, Gibrilla F. Deen, Mustapha S. Kabba, Aiah Lebbie, Ibrahim Franklyn Kamara, Bobson Derrick Fofanah, Anna Maruta, Christiana Kallon, Foday Sahr, Mohamed Samai, Olukemi Adekanmbi, Le Yi, Xuejun Guo, Rugiatu Z. Kamara, Darlinda F. Jiba, Joseph Chukwudi Okeibunor, George A. Yendewa, Emmanuel Firima
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue 1 / 2022
- Published online by Cambridge University Press:
- 07 July 2022, e111
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Objective:
Despite the impact of inappropriate prescribing on antibiotic resistance, data on surgical antibiotic prophylaxis in sub-Saharan Africa are limited. In this study, we evaluated antibiotic use and consumption in surgical prophylaxis in 4 hospitals located in 2 geographic regions of Sierra Leone.
Methods:We used a prospective cohort design to collect data from surgical patients aged 18 years or older between February and October 2021. Data were analyzed using Stata version 16 software.
Results:Of the 753 surgical patients, 439 (58.3%) were females, and 723 (96%) had received at least 1 dose of antibiotics. Only 410 (54.4%) patients had indications for surgical antibiotic prophylaxis consistent with local guidelines. Factors associated with preoperative antibiotic prophylaxis were the type of surgery, wound class, and consistency of surgical antibiotic prophylaxis with local guidelines. Postoperatively, type of surgery, wound class, and consistency of antibiotic use with local guidelines were important factors associated with antibiotic use. Of the 2,482 doses administered, 1,410 (56.8%) were given postoperatively. Preoperative and intraoperative antibiotic use was reported in 645 (26%) and 427 (17.2%) cases, respectively. The most commonly used antibiotic was ceftriaxone 949 (38.2%) with a consumption of 41.6 defined daily doses (DDD) per 100 bed days. Overall, antibiotic consumption was 117.9 DDD per 100 bed days. The Access antibiotics had 72.7 DDD per 100 bed days (61.7%).
Conclusions:We report a high rate of antibiotic consumption for surgical prophylaxis, most of which was not based on local guidelines. To address this growing threat, urgent action is needed to reduce irrational antibiotic prescribing for surgical prophylaxis.
Implementation of surgical site infection surveillance in 16 health facilities in Sierra Leone
- Rugiatu Z. Kamara, Monique Foster, Jamine Weiss, Christiana Conteh
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, p. s63
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Surgical site infections (SSIs) are associated with increased healthcare costs, antibiotic resistance, morbidity, and mortality. In low- and middle-income countries (LMICs), SSIs account for most healthcare-acquired infections (HAIs). In Africa, up to 20% of women who undergo a caesarean section develop a wound infection. Surveillance has been shown to be an essential component in the overall strategy to reduce SSIs. Methods: Surgical site infection surveillance is being implemented in 16 health facilities in Sierra Leone, with at least 1 from each of the 5 US Census regions: Eastern, Western, Northern, Northwestern, and Southern. These health facilities were selected based on the availability of a dedicated infection prevention and control (IPC) focal person. Women were observed for 30 days after caesarean section. A standardized surgical safety and surveillance checklist including case definitions and observable criteria (eg, purulent drainage, wound abscess, or intentional reopening) was used. Clinical staff were trained to collect data and to conduct in-person and phone interviews with patients on days 3, 7, and 30 after caesarean section. Results: From March 2021 to July 2021, a total of 2,529 women had caesarean sections in 15 health facilities; most occurred in the Northern region (785 of 2,529). Among these 2,529 women, 1,522 (60%) had an SSI surveillance checklist started, and of those 1,522, 632 (42%) had a completed checklist. Health facilities in most of the rural regions, (Eastern, Northwestern, and Southern) had no completed checklists. The overall SSI rate for the 15 health facilities was 3% (70 of 2,529). The Southern region had the highest SSI rate at 50% (35 of 70), but the Western region did not report any SSIs. Of the 70 cases, 49 (70%) were identified through active inpatient surveillance and 21 (30%) were identified through postdischarge surveillance. Conclusions: One of the priorities of Sierra Leone’s National IPC Action Plan is to establish HAI surveillance. Surgical site surveillance is an essential component of HAI surveillance and leads to timely identification so infections can be treated quickly. This study was limited by inadequate data collection and patients lost to follow-up after discharge. However, this study illustrates that surveillance leads to the diagnosis of most SSI cases after caesarean section while patients are still hospitalized. Simple yet effective SSI surveillance can be conducted in LMICs to identify and ultimately treat SSI after caesarean section. More support is needed in rural and smaller facilities for better implementation of SSI surveillance in Sierra Leone.
Funding: None
Disclosures: None
The Design and Implementation of an IPC Certificate Course: Experiences From Sierra Leone
- Jamine Weiss, Amy Kolwaite, Meghan Lyman, Getachew Kassa, Miriam Rabkin, Anna Maruta, Marita Murrman, Hassan Benya, Christiana Conteh
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, p. s498
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Trained infection prevention and control (IPC) practitioners are critical to reducing healthcare-associated infections (HAI) and improving patient safety. Despite having HAI rates 3 times higher than high-income countries, many low- and middle-income countries (LMICs) lack trained IPC professionals. During the 2014–2016 Ebola outbreak in West Africa, the Sierra Leone Ministry of Health and Sanitation (MoHS) recognized this need and appointed and trained IPC focal persons at all district hospitals. Following the outbreak, MoHS requested assistance from the US CDC to develop and implement a comprehensive IPC training program for IPC specialists. Methods: The CDC, alongside its partners, convened a multidisciplinary team to develop an IPC certificate course. ICAP led the curriculum development process using a “backwards design” approach, starting with development of competencies and learning objectives, then designing an evaluation framework and learning strategies, and finally, identifying course content. The curriculum was based on existing resources, primarily designed for high-income countries, which were adapted to the Sierra Leone context and aligned with national IPC policies and guidelines. Additionally, an IPC steering committee, led by MoHS, was established to provide national leadership and oversight and make country-level decisions regarding accreditation and career pathways for IPC specialists. Results: The course includes three 2-week workshops over 6 months consisting of classroom didactics and hands-on activities. Topics include standard and transmission-based precautions, microbiology, laboratory, HAI, quality improvement, leadership, and scientific writing. Between sessions, participants conduct IPC activities at their work site and share results during subsequent workshops. Participants receive electronic tablets, which contain course content, assessment tools, and references, to upload their work into a cloud-based storage system for facilitators to provide feedback. They also receive in-person mentorship and connect with peers through a group messaging platform to share lessons learned. Participants’ knowledge and skills are assessed using a before-and-after test and observing them perform IPC practices using standardized checklists. The first cohort of 25 participants will complete the course in November 2019. Conclusions: The IPC certificate course is the first comprehensive, competency-based IPC training in Sierra Leone. Successes, challenges, sustainability, and lessons learned remain to be determined; however, based on similar models, the course has the potential to significantly improve IPC in Sierra Leone. Additionally, it is a model that can be replicated in other resource-limited settings.
Funding: None
Disclosure:None
Road to Increasing AMR: A Study on Antibiotics Prescribing Pattern
- Bobson Derrick Fofanah, Christiana Conteh, Jamine Weiss
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s496-s497
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Infectious diseases and the rapid emergence of multidrug-resistant pathogens continue to pose a threat to global health. The development of antimicrobial-resistant organisms is an alarming issue caused by inappropriate use of antibiotic agents. It is estimated that death from antimicrobial resistant pathogens could increase >10-fold to ~10 million deaths annually by 2050 if action is not taken. “It is essential to have reliable data on how medicines are used in order to identify areas to develop targeted interventions” (WHO 2011). Investigating antimicrobial use in hospitals is the first step in evaluating the underlying causes of AMR. In Sierra Leone, no other study related to antibiotic prescribing patterns in hospital setting has been undertaken. Objective: To investigate antibiotic prescription patterns using the WHO hospital antimicrobial use indicator tool at the Kingharman Hospital for 1 month. Methods: Data were collected from patient charts for 1 month, January 1–31, 2019. A data extraction tool was used to capture information on patient demographics, diagnosis, and antibiotics prescription details regarding dosage, duration, and frequency of administration. The tool adopted 6 selected indicators from the WHO antimicrobial use manual to measure the extent of antibiotic use in hospital and performance among prescribers. Results: Of the 189 charts reviewed, 175 included antibiotic prescriptions. The percentage of prescriptions involving antibiotics was 92.5%. The average number of drugs prescribed was 2, with an average duration of 5.2 days. Moreover, 50.5% of antibiotics prescribed were generic, and 96.6% were from the Ministry of Health and Sanitation Essential Medicine List (EML). The most commonly used antibiotics were ciprofloxacin (38.8%), followed by ceftriaxone (23.0%), amoxicillin (16.8%), metronidazole (8.5%), and others(12.7%). Typhoid accounted for 34.8% of broad-spectrum antibiotics, UTI accounted for 17.7%, malaria accounted for 12.5%, 25.5% were unspecified, and 9.5% were for unclear diagnoses. Typically, combinations of fluroquinolones and cephalosporins were used to treat typhoid and UTIs. Conclusions: This cross-sectional study represents a broad picture of antibiotic prescribing patterns at the King Harman Hospital. There was no strict adherence to the WHO recommended prescribing guidelines. These findings also indicate the degree of irrational and inappropriate prescribing of broad-spectrum antibiotics. This study highlights the need for a comprehensive assessment of antimicrobial use to gain a better understanding of national antibiotic use and to guide interventions to reducing AMR.
Funding: None
Disclosures: None
If I am discussing specific healthcare products or services, I will use generic names to extent possible. If I need to use trade names, I will use trade names from several companies when available, and not just trade names from any single company.
Disagree
Christiana Kallon
Patient Involvement in Infection Prevention and Control (IPC) Practice: Knowledge and Perception Study
- Bobson Derrick Fofanah, Christiana Conteh
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, p. s493
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Patient involvement is increasingly recognized as critical component for improved care, and patients has been identified of as having a potentially important role for better health outcome as a result of their involvement in their care plan. A usual saying that infection prevention and control is “everyone’s business” is frequently understood to include not only healthcare workers but also patients and their relatives, all of whom are seen as stakeholders with a part to play in ensuring a better patient outcome. There is limited evidence about knowledge and perception about involving patient and/or relatives in IPC implementation in a post–Ebola-outbreak country. Objectives: We aimed to ascertain the knowledge and perception of patient involvement in infection prevention and control (IPC) practice. Methods: We used a qualitative approach comprising interviews with patients and/or relatives and health workers sampled from 5 hospitals. Participants (n = 60) included 25 nurses, 25 patients and/or relatives, 5 IPC focal persons, and 5 hospital administrators. Interviews used a structured questionnaire to explore staff views on patient involvement. A separate questionnaire was used to survey patient perspectives and knowledge about basic hospital IPC practices. Results: Of 60 interviews, 64% of nurses supported involving patient in hospital IPC practice, saying that the patient can serve as a reminder during the time of care, whereas 36% disagreed with involving the patient because of fear of having confrontations with the patient. Also, 92% of patients and/or relatives agreed to their involvement because they viewed it as their right; only 8% did not accept involvement because they thought it was a burden and not their responsibility. All 5 IPC focal persons (100%) supported patient involvement; they thought it would enhance overall IPC compliance and keep healthcare workers reminded of IPC practice, most especially hand hygiene. Also, 100% of hospital administrators supported involving patients because they felt that patient should be involved in their care plan. Conclusions: From this study, it is evident that patient involvement is key in optimizing IPC compliance in hospitals. The study findings indicate that most patients have knowledge of the importance of hand washing since the Ebola outbreak; however, they lack knowledge on other practices such as waste disposal, cough etiquette, etc. There is need for IPC orientation on admission and continuous patient education.
Funding: None
Disclosures: None
If I am discussing specific healthcare products or services, I will use generic names to extent possible. If I need to use trade names, I will use trade names from several companies when available, and not just trade names from any single company.
Disagree
Christiana Kallon
Feasible Surgical Site Infection Surveillance in Resource-Limited Settings: A Pilot in Sierra Leone
- Matthew Westercamp, Aqueelah Barrie, Christiana Conteh, Danica Gomes, Hassan Benya, Jamine Weiss, Anna Maruta, Rachel Smith
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, p. s38
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Surgical site infections (SSIs) are among the most common healthcare-associated infections (HAIs) in low- and middle-income countries (LMICs). SSI surveillance can be challenging and resource-intensive to implement in LMICs. To support feasible LMIC SSI surveillance, we piloted a multisite SSI surveillance protocol using simplified case definitions and methodology in Sierra Leone. Methods: A standardized evaluation tool was used to assess SSI surveillance knowledge, capacity, and attitudes at 5 proposed facilities. We used simplified case definitions restricted to objective, observable criteria (eg, wound purulence or intentional reopening) without considering the depth of infection. Surveillance was limited to post-cesarean delivery patients to control variability of patient-level infection risk and to decrease data collection requirements. Phone-based patient interviews at 30-days facilitated postdischarge case finding. Surveillance activities utilized existing clinical staff without monetary incentives. The Ministry of Health provided training and support for data management and analysis. Results: Three facilities were selected for initial implementation. At all facilities, administration and surgical staff described most, or all, infections as “preventable” and all considered SSIs an “important problem” at their facility. However, capacity assessments revealed limited staff availability to support surveillance activities, limited experience in systematic data collection, nonstandardized patient records as the basis for data collection, lack of unique and consistent patient identifiers to link patient encounters, and no quality-assured microbiology services. To limit system demands and to maximize usefulness, our surveillance data collection elements were built into a newly developed clinical surgical safety checklist that was designed to support surgeons’ clinical decision making. Following implementation and 2 months of SSI surveillance activities, 77% (392 of 509) of post-cesarean delivery patients had a checklist completed within the surveillance system. Only 145 of 392 patients (37%) under surveillance were contacted for final 30-day phone interview. Combined SSI rate for the initial 2-months of data collection in Sierra Leone was 8% (32 of 392) with 31% (10 of 32) identified through postdischarge case finding. Discussion: The surveillance strategy piloted in Sierra Leone represents a departure from established HAI strategies in the use of simplified case definitions and implementation methods that prioritize current feasibility in a resource-limited setting. However, our pilot implementation results suggest that even these simplified SSI surveillance methods may lack sustainability without additional resources, especially in postdischarge case finding. However, even limited phone-based patient interviews identified a substantial number of infections in this population. Although it was not addressed in this pilot study, feasible laboratory capacity building to support HAI surveillance efforts and promote appropriate treatment should be explored.
Funding: None
Disclosures: None
Point-Prevalence Survey on Antibiotics Use in Six Regional Hospitals in Sierra Leone
- Ralph Williams, Christiana Conteh, Joseph Sam Kanu
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, p. s494
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Antibiotic resistance (AMR) is a safety concern for patients in Sierra Leone. AMR can occur in communities and as well in the process of receiving treatments in healthcare settings, and it can pose a major threat to patient safety. Healthcare-associated infections and AMR result in longer duration of illness, longer treatment, higher mortality, increased costs, and increased burden to health facilities. Objective: The purpose of this study was to generate more reliable estimates of the risk factors for the prevalence of HAI and to investigate patterns of antibiotic prescriptions done. Methods: The survey was conducted in 6 regional hospitals in Sierra Leone (Kono, Kambia, BO, Makeni, Moyamba, and Kenema) from June 16 to July 10 2019. The survey targeted inpatients in the pediatric, maternity, medical, and surgical wards. A structured questionnaire adopted from the WHO PPS form was used to collect information from patient medical charts and care notes. Results: Data were collected from 156 patients, of whom 140 patients were on antibiotics, 100 were women, and 40 were men. Patients on 1 antibiotic regimen accounted for 8.6% (n = 12) and 91.4% (n = 128) on a regimen of 2 or 3 antibiotics. Only 5 patients (3.6%) were on oral antibiotics and 135 (96.4%) were on IV antibiotics. In the maternity ward, 28 of 40 patients (70%) had had a caesarian section and were on 2 or more antibiotics; 18 patients with caesarian sections (64.3%) developed complications and continued on an antibiotic regimen for >1 week. The remaining 12 patients (30%) in the maternity ward were admitted for anemia and hypertension (ie, preeclampsia), and these patients were on 1 antibiotic regimen for which they had no clinical indication. Conclusions: The survey results show that every patient admitted to the hospital was covered with antibiotics with or without indications; no laboratory investigations were performed before antibiotics were initiated. These findings further reveal a large number of patients who were exposed to intravenous cannulation, which predisposes catheter-associated bloodstream infections. The survey results justify the need for an antibiotic stewardship program to guide use of antibiotics.
Funding: None
Disclosures: None
If I am discussing specific healthcare products or services, I will use generic names to extent possible. If I need to use trade names, I will use trade names from several companies when available, and not just trade names from any single company.
Disagree
Christiana Kallon
Status of Infection Prevention and Control in Selected Hospitals in Sierra Leone
- Anna Maruta, Christiana Conteh, Ralph Williams
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s497-s498
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Improved infection prevention and control (IPC) reduces healthcare-associated infections (HAIs). Following the Ebola virus disease (EVD) outbreak in West Africa (2014–2016), Sierra Leone made substantial investments in strengthening IPC in health facilities. The WHO identified 8 core components of IPC and developed an accompanying assessment framework (IPCAF) to monitor IPC capacity and progress. The IPCAF reflects the 8 WHO core components of IPC. The core component constitute a consistent universal outline that supports guidance to healthcare decision makers and service providers at national and international levels. We conducted an in-depth assessment of IPC practices in Sierra Leone using the IPCAF tool. Methods: This assessment was conducted in in July 2019 over a 2-week period. Data were collected through interview with IPC focal persons as well as observations and corroboration of document and immediate feedback on findings given to facilities through brief exit meetings. All areas of the facility were assessed (ie, all wards, operation theatres, laboratories maternity units, sterile service departments, waste management units, etc). The main objective was to identify the gaps and challenges faced by health facilities. Each component was scored based on the responses and observations, with the scores ranging from zero to 100 and the maximum score was 800. The IPCAF allocated hospitals to 4 different “IPC levels”: inadequate, basic, intermediate, and advanced. Results: Moreover, 13 hospitals were assessed, including 12 primary level hospitals and 1 secondary level hospital. The median score was 367. 5 (IQR, 110), which corresponds to a basic level of IPC. Primary-level hospitals scored higher (median, 373; IQR, 112.5) compared to secondary-level hospitals (median, 280; IQR, 0). The lowest score was in healthcare-associated infection surveillance (median, 0; IQR, 5), and the highest score was in the built environment, availability of materials, and equipment to support IPC (median, 62.5; IQR, 22.5). Conclusions: The assessment provides a baseline of the status of IPC in Sierra Leone in the post-EVD period using the IPCAF tool. These results can be used to guide healthcare facilities and policy makers in developing strategies for IPC quality improvement projects to improve low-performing healthcare facilities. Significant gaps were observed in key IPC areas, especially in secondary-level health facilities. There is need to establish national surveillance for healthcare-associated infections, to institutionalize monitoring of IPC practices, and to ensure an appropriate staffing–workload ratio in health facilities.
Funding: None
Disclosures:
If I am presenting research funded by a commercial company, the information presented will be based on generally accepted scientific principals and methods, and will not promote the commercial interest of the Funding: company. Disagree
Anna Maruta
If I am discussing specific healthcare products or services, I will use generic names to extent possible. If I need to use trade names, I will use trade names from several companies when available, and not just trade names from any single company.
Disagree
Christiana Kallon




